Sunday, May 24, 2009
What is a “surplus lines insurer” and what does that have to do with the safety of HMSA’s new online service?
by Larry Geller
I was wondering why a doctor would risk a precious medical license by participating in this on-line service. Towards the end of this article I’ll explain what I learned. And thanks to the person who sent the “leak.”
On an impulse, I wrote a letter to the editor of the Advertiser. It appeared in today’s paper, a great spot. Here’s what I wrote:
HMSA ONLINE CARE
PROMOTING SERVICE AS SUBSTITUTE UNWISE
Sen. Josh Green is correct in objecting to HMSA's misplaced recommendation of its online consultation service (Advertiser, May 21).
With some possible exceptions, the quality of the consultation does not adequately protect the patient. The online doctor can't look down your throat or in your ear, for example, and so the care that can be given is very limited. It remains to be seen whether patients will learn to make only appropriate use of online consultations.
There is a better alternative to visiting the ER — do what the tourists do, where possible — visit an after-hours walk-in clinic. On rare occasions when something needed immediate attention, our family did just that. A live doctor was able to provide top-notch medical care.
Our Department of Health could promote the availability of walk-in clinics as part of a comprehensive healthcare solution for Hawai'i. HMSA's promotion of its online service as a substitute for a visit to a flesh-and-blood doctor is irresponsible.
The service could become a useful adjunct to treatment if a patient's primary care physician is participating in the experiment, and of course could answer general questions authoritatively, or assist those too remote to have any other option.
Larry Geller
Honolulu
The original Advertiser article reports that HMSA does promote their on-line service as an alternative to an office visit:
HMSA has said the system isn't a replacement for face-to-face office visits and may be attractive to people who haven't had the time to make a doctor's appointment. Moreover, it sees the program as being an alternative to the 90,000 annual emergency room visits that are costly, but sometimes occur because no doctor's offices are open.
It’s doublespeak. Sounds like they are promoting the service for those “who haven't had the time to make a doctor's appointment” as a replacement for a face-to-face visit, doesn’t it? And again, there are other ways to reduce the number of ER visits if the state cared to do that.
Rep. Green wrote in that Advertiser article:
"It is deeply irresponsible and reckless for HMSA to use the swine flu crisis to promote Online Care in their recent announcements, which falsely imply that it is safer for a patient in Hawai'i to use the Online Care system than to see a doctor in person," Green, a sometime HMSA critic, said in an e-mail.
"These assertions are medically unsound and undermine the professional standard of care established by the medical community in Hawai'i."
Of course, if HMSA can replace office visits with on-line sessions, since a responsible doctor won’t prescribe treatment this way (IMHO), HMSA will save a fortune. That’s right, if you don’t see a doctor in person and get your strep throat diagnosed, they won’t have to pay to treat it, will they.
Check out the web promotion. These are snipped from HMSA’s website for educational purposes only. Click for large enough to read.
Ok so far, maybe. Let’s learn more:
Some of this sounds really good! Choose a physician based on language, qualifications. Cool. It says you can get treatment and a prescription. The physician will inform your regular doctor about what was prescribed for you. It doesn't say when, but that’s a quibble. You could have something growing in you that needs to be taken out, but of course the on-line doctor can’t press your abdomen to discover that.
Why would a qualified physician be participating in a service where the patient’s blood pressure can’t even be checked? Where a patient might want an antibiotic, for example, and give a fake report just to get the meds?
The rates may look attractive, compared with your co-pay right now, as the chart below indicates, but keep in mind that you’re not getting a “real” doctor visit for your money, and you won’t be able to talk as long as your issue may require. The doctor can’t look down your throat if necessary. Even if you have a webcam, it won’t work. And notice that HMSA is selling this to non-members, so someone with no insurance is going to pay for an inferior level of service—that could cost them their life, if they don’t follow up with an office visit. Or, if the doctor is responsible, will be useless. Get thee to a real physician is what the on-line doctor better say. $45 please.
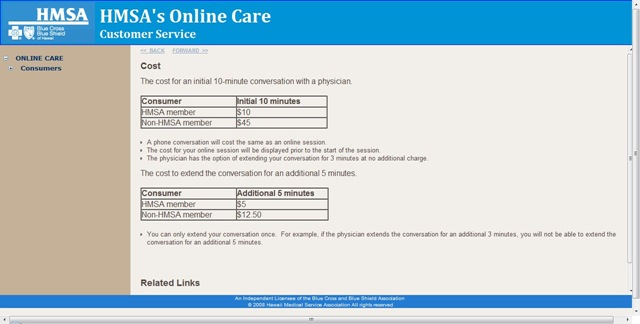
HMSA will determine, apparently without recourse, how long you can talk with your on-line physician. If the physician has extended the talk (by 3 minutes!) it cannot be extended again. HMSA has spoken. Doesn’t matter if you and your physician need to talk more.
This is a great example that critics of managed care can use to show that insurers are getting between physicians and their patients.
Why would a doctor agree to risk a precious medical license in order to participate in this plan? Here’s why: HMSA provides them with insurance. From the doctor’s brochure:
Is malpractice coverage included with HMSA’s Online Care?
Yes. Malpractice coverage is provided by the Lexington Insurance Company (a member company of AIG), the largest medical malpractice carrier in the country. The policy is independent of your existing malpractice coverage for your practice.
Disclaimer: This product description is for informational purposes only and does not provide a complete description of coverage terms, conditions, exclusions and limits. Insurance for this program may be provided by a surplus lines insurer.
So the online doc is covered (not you). “But what,” you may ask, “is a ‘surplus lines insurer?’ “
From the first Google hit:
There are some cases, however, (generally less than 10% of policies nationwide) where the licensed insurers will not accept a risk because it does not meet their internally established guidelines. The risk may be too big, too unusual or substandard. In these cases, a specially licensed producer called a surplus line producer gets involved. Their special surplus line license allows them to procure a policy for you from an insurer that is not licensed in your state.
Much of Hawaii’s malpractice insurance comes from out of state anyway. There are reasons for this that are too lengthy to go into here. I am concerned, of course, about this part: “The risk may be too big, too unusual or substandard.”
Given the uniqueness of this program, perhaps that’s what HMSA has to do. But remember, the insurance protects the doctor facing you on the screen. If you are injured or harmed in some way because you participated, and if you live, you have to sue. Also, many doctors and the Hawaii Medical Association are pushing hard in the state legislature to limit what you can recover as damages (they call it “tort reform”). Should they succeed one day, a patient’s ability to recover damages would be severely limited. But the participating doctor is covered.
That would explain why the face you see on the screen is smiling.
Most of a doctor’s time is taken up with questions the patient has and/or for checkups or exacerbations of chronic conditions. In many cases a patent has already seen a doctor for the condition and the examining doctor has the patients chart at hand. And, of course, when a physical exam is indicated a doctor will tell a tele-med patient that and require they come in for an office visit.
But that is rare. Most office visits are educational in nature. And most conditions are diagnosed based on what the patent tells the doctor verbally. Many times a patient may not come in for a visit because it’s a huge hassle but with tele-med they may call in and find out it is serious enough to come in whereas otherwise they might let it go until it’s “too late”.
The need to “look down your throat” is usually to make the patient feel like you’re doing something about their cold or flu- which is usually viral and doesn’t require treatment. If you’re complaining about a sore throat it’s going to be red when the doc looks at it. If you have chest congestion your breath sounds are going to be gravelly. Odds are people aren’t going to be lying about their symptoms and they can just easily do that in an office visit if they are so inclined.
That “throat culture” you mention is almost never- and never “automatically”- done when the patient first presents. In fact is discouraged when there is a complaint of a cold or flu. They detect bacterial infections only.
Most bacterial infections are secondary to a viral one – the come after a viral cold has weakened the patient and cause them to be susceptible to a bacterial infection. That’s why doctors are reluctant to give out antibiotics (or take “throat cultures”) and only do so if patients demand them over the doctor’s objections or they have not gotten better after a few days to a week.
If an office visit in needed the doctor will tell the patient that. But for the 90% of cases where it isn’t, tele-med is great for patients and doctors.
As to whether they touch, my experience is different. Two of my doctors do. One found something. I had abdominal surgery a couple of years ago to yank it out, and a good thing, too.
So maybe it's a case of "your mileage will vary," but keep in mind that the telemedicine doc, unless you've been issued one of those fancy Japanese toilet seats, can't tell much about you, and can't even really hear if your chest is congested or your voice is gravelly. And then the coin drops, and HMSA won't even let you talk anymore. Nope, not for me, anyway.
Links to this post:
<< Home









Post a Comment